Knee Replacement Surgery In Singapore: Procedure and Recovery
Home / Conditions We Treat / Total Knee Replacement Surgery in Singapore
Total knee replacement surgery is a procedure designed to relieve pain and restore mobility in patients with severe knee joint damage, often caused by osteoarthritis or injury. During the procedure, the damaged surfaces of the knee joint are replaced with artificial components to improve function and quality of life. An experienced orthopedic specialist evaluates each case to determine a suitable surgical approach and rehabilitation plan.
This information is aligned with MOH surgical guidelines and standards, which ensure that procedures performed in Singapore meet established safety and clinical care requirements.
What is Knee Replacement Surgery?

People whose knees are severely damaged by arthritis or injury may have difficulty performing simple activities such as walking or climbing stairs. They might even experience pain when sitting or lying down. In some cases, altered movement patterns caused by related joint conditions, such as ankle arthritis, can place additional strain on the knees over time. When nonsurgical treatments such as medication and walking aids are no longer helpful, total knee replacement surgery may be considered in Singapore. This procedure can help relieve pain, correct leg deformities, and enable patients to resume daily activities with improved mobility.
Developments in surgical materials and techniques have contributed to more consistent outcomes in knee replacement surgery in Singapore over time. Today, the procedure is commonly performed in many hospitals, with reported success rates of around 95 per cent in appropriately selected patients.
The following information provides an overview of the procedure’s complexity, whether you are already preparing for surgery or exploring possible treatment options. It is important to note that knee replacement surgery might not always be the most suitable solution for every patient. Consulting a knee doctor in Singapore can help determine the most appropriate approach based on your condition and lifestyle needs.
Let’s take a look at the various causes behind knee-related problems.
Understanding the Knee as an Important Part of the Body

To understand knee replacement surgery better, it is vital to understand the knees and their function in the human body. The knees, as the body’s largest joint, support our weight and allow us to move. Therefore, having healthy knees is necessary for performing most everyday activities.
The knee is formed by three parts — the lower end of the thigh bone (femur), the upper end of the shinbone (tibia) and the kneecap (patella). The ends of these bones are covered with articular cartilage, a smooth substance that protects the bones and enables them to move easily within the joint. Between the femur and tibia are menisci, C-shaped wedges that cushion the joint by acting as ‘shock absorbers’. The femur and tibia are held together by large ligaments that give stability. The long thigh muscles also help to strengthen the knees. The remaining surfaces of the knee are covered by a thin coating called the synovial membrane. In a healthy knee, this membrane releases a fluid that lubricates the cartilage and reduces friction. In most cases, all of these elements work in unison. Disease or injury, on the other hand, can upset this balance, resulting in muscle weakening, discomfort, and impaired function. When this happens, total knee replacement surgery may be recommended to relieve pain and improve mobility.
Common Causes of Knee Injuries
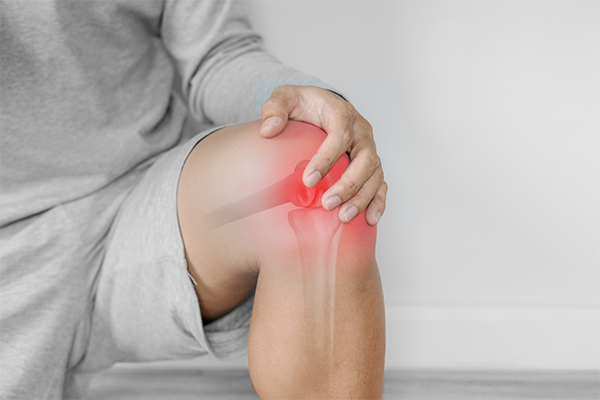
The most common cause of chronic knee pain and impairment is arthritis. As arthritis causes the knees to wear out, the most common treatment is knee replacement surgery. Although there are several varieties of arthritis, these three are the most common: osteoarthritis, rheumatoid arthritis, and post-traumatic arthritis. In some cases, knee pain or instability may also result from ligament injuries that require specialised care, such as ACL surgery, to restore strength and joint stability.
Osteoarthritis
Osteoarthritis is an age-related “wear and tear” kind of arthritis. The cartilage that cushions the bones of the knee softens and wears away. This results in the bones rubbing against one another, causing knee pain and stiffness. Bone spurs are a common symptom of osteoarthritis. Although it typically occurs in people 50 years old and above, it may also occur in younger people.
Rheumatoid arthritis
Rheumatoid arthritis is the most common form of a group of disorders known as “inflammatory arthritis”. It is a disease in which the synovial membrane surrounding the joint becomes inflamed and thickened. This chronic inflammation can damage the cartilage and eventually cause cartilage loss, pain and stiffness.
Post-traumatic arthritis
Post-traumatic arthritis can occur following a severe knee injury. Fractures of the bones that surround the knee or tears of the knee ligaments may cause damage to the articular cartilage over time. As a result, the knee function is limited and pain will be felt.
What is knee replacement surgery?

A knee replacement surgery, also known as knee arthroplasty, is more accurately described as a “resurfacing” procedure because only the damaged surfaces of the bones are replaced rather than the entire joint. An experienced knee specialist evaluates each case to determine the most suitable surgical approach based on the extent of joint damage and the patient’s condition.
A knee replacement surgery is consist of four basic steps:
Step 1: Preparation of the bone. Firstly, the damaged cartilage surfaces at the ends of the femur and tibia are removed, along with a small amount of underlying bone.
Step 2: Positioning the metal implants. Secondly, the removed cartilage and bone are replaced with metal components that recreate the surface of the joint. These metal parts may be cemented or “press-fit” into the bone.
Step 3: Resurfacing the patella. Next, the undersurface of the patella (kneecap) is cut and resurfaced with a plastic button. Depending on the case, certain surgeons do not resurface the patella.
Step 4: Insertion of a spacer. Lastly, a medical-grade plastic spacer is inserted between the metal components to create a smooth gliding surface.
Is knee replacement surgery applicable for you?
Total knee replacement surgery has no absolute weight or age constraints. Despite the fact that the majority of persons who undergo this treatment are between the ages of 50 and 80, surgical recommendations are based on a patient’s pain and disability rather than their age. As a result, orthopaedic surgeons are able to and have successfully conducted this procedure on patients of various ages.
When is knee replacement surgery recommended?
There are multiple instances when knee replacement surgery may be recommended. Below are some symptoms of patients who may benefit from total knee replacement:
- Moderate to severe knee pain while resting, either in the day or at night
- Severe stiffness or knee pain that limits everyday activities such as walking, climbing stairs, and getting on and off chairs.
- Knee deformity — a bowing in or out of the knee
- Chronic knee inflammation and swelling that does not improve with medications or rest
- No significant improvement with other treatments such as physical therapy, anti-inflammatory medications, lubricating injections, cortisone injections, or other surgeries
Before proceeding, patients are evaluated according to the MOH standards for surgical safety to ensure that the procedure is appropriate and carried out under regulated clinical protocols designed to minimise risk and promote optimal recovery.
How Is An Orthopaedic Evaluation For Knee Replacement Surgery Carried Out?
An orthopaedic evaluation must be done before conducting the surgery. It consists of the following steps:
1. Inquiry into the patient’s medical history in order to learn more about the patient’s overall health and the severity of the knee pain and ability to function.
2. A physical examination to assess the range of motion, stability, strength, and general leg alignment of the knees.
3. X-rays to determine the severity of the damage and deformity in the knee.
4. Other tests such as blood tests or advanced imaging, such as a magnetic resonance imaging (MRI) scan might be needed to evaluate the condition of the bone and soft tissues in the knee.
After reviewing the evaluation results, the orthopaedic surgeon will discuss the range of treatment options with the patient. These include physical therapy, injections, medications, and total knee replacement surgery. If surgery is determined to be the most suitable option to relieve pain and improve function in the knee, the risks and complications will be discussed with the patient as well. Such risks and complications include those related to the surgery itself and those that may occur over time post-surgery.
The following should be discussed with the surgeon before the knee replacement surgery:
Anaesthesia
Upon arriving at the hospital or surgery centre, the patient will be evaluated by a member of the anaesthesia team. The most common kinds of anaesthesia are general (where one is put to sleep), spinal, epidural or regional block anaesthesia (where one is awake but the body is numb from the waist down). Taking the patient’s input into consideration, the anaesthesia team will determine the most suitable form of anaesthesia for knee replacement surgery.
Procedure
Typically, the surgical procedure will take about 1 to 2 hours. First, the orthopaedic surgeon will remove the damaged cartilage and bone. Next, the new metal and plastic implants are positioned to restore the alignment and function of the knee. Depending on the individual’s needs, different kinds of knee implants are used.
After the procedure, the patient will be moved to the recovery room. They will remain there for several hours while the recovery from anaesthesia is monitored. Once the patient has woken up, they will be taken to their hospital ward or discharged home.
Are there possible complications when getting knee replacement surgery?

The complication rate following a total knee replacement surgery is generally low. Severe complications like knee joint infection occur in less than 2% of patients. Furthermore, major medical complications such as a heart attack or stroke occur even less often. However, chronic illnesses may increase the risk of complications occurring. Although uncommon, when such complications occur, full recovery can be prolonged or limited. In line with the MOH patient safety guidelines, patients are advised to thoroughly discuss their concerns with an orthopaedic surgeon before surgery.
Infection
Infection may occur in the wound or deep around the prosthesis. This can happen within days, weeks or even years after the knee replacement surgery. Generally, minor infections in the wound area are treated with antibiotics. As for major or deep infections, they may require more surgery and removal of the prosthesis. Furthermore, any infection in the body can spread to the joint replacement.
Blood clots
One of the most common complications of knee replacement surgery is blood clots in the leg veins. Although blood clots can occur in any deep vein, they most commonly form in the veins of the pelvis, calf, or thigh. These clots can potentially become life-threatening if they break free and travel to the lungs. A prevention program will be outlined by the surgeon, which may include medication to thin the blood, periodic elevation of the legs, lower leg exercises to increase circulation and support stockings.
Implant problems
Even when surgical procedures, implant materials, and designs evolve, implant surfaces and components may still wear down and loosen. Furthermore, though a range of motion of 115 degrees is normally predicted following surgery, scarring of the knee can occur. As a result, motion may be restricted, especially in patients who already had restricted motion prior to surgery.
Continued pain
A small fraction of patients have reported experiencing continued pain after a knee replacement surgery. However, this complication is rare as most patients experience great pain relief post-surgery.
Neurovascular injury
Although this is rare, injury to the nerves or blood vessels around the knee can occur during surgery.
How To Prepare For A Knee Replacement Surgery in Singapore
Preparing for a knee replacement surgery involves understanding the procedure, planning for recovery, and following your surgeon’s preoperative instructions. Patients are advised to undergo a medical evaluation, adjust certain medications, and prepare their homes for post-surgery mobility. Maintaining a balanced diet, engaging in light preoperative exercises, and arranging for assistance during the recovery period can also support smoother rehabilitation.
Those seeking care at our Mount Elizabeth Novena orthopaedic clinic can discuss personalised preparation steps with their orthopaedic specialist to ensure the procedure and recovery are managed according to individual health needs.

Medications
Current medications taken by the patient will be discussed with the orthopaedic surgeon. The patient will then be advised on which ones to stop taking before the surgical procedure.
Dental evaluation
Even though the incidence of infection after knee replacement surgery is very low, an infection can occur if bacteria enter the bloodstream. Therefore, to lower the risk of infection, major dental procedures, such as tooth extractions and periodontal work, should be completed before total knee replacement surgery.
Urinary evaluations
Patients who have a history of recent or frequent urinary infections should undergo a urological evaluation before surgery. Older men with prostate disease, especially, should consider completing the required treatment before undergoing knee replacement surgery.
Social planning
Even though one will be able to walk with crutches, a cane or a walker after knee replacement surgery, help will probably be needed to accomplish certain tasks. These can include bathing, cooking, shopping and doing laundry.
If the patient lives alone, a discharge planner or social worker at the hospital can help to make advance arrangements for some assistance at home. Alternatively, a short stay in an extended care facility during recovery can also be arranged.
Home planning
There are several changes that one can make to their home in order for easier navigation during the recovery process. The modifications below may help make everyday activities easier:
If the house is a multi-storey one, a temporary living space on the same floor can help because walking up and down stairs can be difficult during the initial stages of recovery. Additionally, you can take care of the following:
- Removing all loose carpets and cords
- A stable chair during the early stages of recovery with a firm seat cushion and back, a height of 18 to 20 inches, two arms, and a footstool for intermittent leg elevation
- Secure handrails along the stairways
- Secure handrails or safety bars in the shower or bath
- A stable shower bench or chair for bathing
- A toilet seat riser with arms if one has a low toilet
What should one expect during their stay at the hospital?

If admitted, the patient will probably stay in the hospital for one to three days.
Pain management
After surgery, it is normal to feel some pain. This is a natural part of the recovery process. The doctor and nurses will work to ease the pain, which can help to speed up the healing.
Normally, medications are prescribed for short-term pain relief after surgery. There are several kinds of medicines available to help manage pain. These include local anaesthetics, acetaminophen, nonsteroidal anti-inflammatory drugs (NSAIDs) and opioids. A combination of these medications may be used to improve pain relief and minimise the need for opioids.
One should be aware that even though opioids help to relieve pain post-surgery, they are a narcotic and can be addictive. In fact, opioid dependency and overdose have become a major public health issue in the U.S. Therefore, it is crucial to use opioids only as directed by one’s doctor. The usage of opioids should be stopped as soon as the pain begins to improve. If it has not begun to improve within a few days post-surgery, one should consult their doctor.
Blood clot prevention
In order to prevent blood clots and decrease leg swelling, one or more measures may be prescribed by the surgeon. These can include blood thinners, inflatable leg coverings (compression boots) and special support hose.
Additionally, foot and ankle movement is encouraged immediately after surgery to increase blood flow in the leg muscles. This will in turn help to prevent leg swelling and blood clots.
Physical therapy
Majority of patients will be able to begin exercising their knee hours after surgery. A physical therapist will teach specific exercises to strengthen the leg and restore knee movement to allow walking and other everyday activities soon after the operation.
To further restore movement in the knee and leg, the surgeon may use a knee-supporting device called a continuous passive movement (CPM) exercise machine. This device slowly moves the knee while the patient is in bed. Although there is no evidence yet to show that these machines improve outcomes, certain surgeons believe in its benefits. It is perceived to decrease leg swelling by elevating the leg and improve blood circulation by moving the muscle of the leg.
Preventing pneumonia
Shallow breathing in the early postoperative period is not uncommon in patients. This is normally because of the effects of anaesthesia, pain medications and prolonged time spent in bed. As a result of shallow breathing, a partial collapse of the lungs, known as atelectasis, can occur. This can make patients susceptible to pneumonia. To help prevent this, it is crucial to take frequent deep breaths. A simple breathing apparatus called a spirometer may be provided to encourage deep breathing.
What should one expect during their recovery at home?

The surgical outcomes are dependent on how well the orthopaedic specialist’s instructions are followed in the first few weeks after surgery at home.
Wound care
The patient will either have stitches or staples running along the wound or a suture beneath the skin on the front of the knee. While a suture beneath the skin does not require removal, stitches or staples will be removed several weeks post-surgery.
One should refrain from soaking the wound in water until it has fully sealed and dried. The wound may be bandaged to prevent irritation from support stockings or clothing.
Diet
It is common for there to be some loss of appetite for several weeks post-surgery. It is essential to maintain a balanced diet, usually with an iron supplement, to help the wound heal and restore muscle strength.
Activity
A crucial portion of home care is exercise, especially during the first few weeks post-surgery. One should be able to resume most everyday activities after 3 to 6 weeks, although some pain at night and with activity is not uncommon.
Physical therapy is helpful in restoring movement and function. An effective activity program should include the following:
- Specific exercises several times a day to restore movement and strengthen the knee. The exercises should be able to be done without help, but one may have a physical therapist help them at home or in a therapy centre the first few weeks post-surgery.
- Resuming normal everyday household activities such as sitting, standing, and climbing stairs
- A graduated walking program to slowly increase mobility, initially at home and later outside
Most patients are able to go back to driving about 4 to 6 weeks post-surgery. Driving can probably be resumed when the knee is able to bend enough to enter and sit comfortably in the car. Muscle control should also provide enough reaction time for braking and accelerating.
How can one avoid problems after total knee replacement surgery?
Recognizing the signs of a blood clot
The orthopaedic surgeon’s instructions should be followed carefully to reduce the risk of blood clots developing during the initial weeks of recovery. The continuation of blood-thinning medications may be recommended. It is important to notify one’s doctor if any of the following warning signs are developed.
Warning signs of blood clots
The warning signs of possible blood clots in the leg can include the following:
- New or increasing swelling in the calf, ankle, and foot
- Increasing pain in the calf
- Pain or tenderness above or below the knee, often described as a cramp
- Reddish or bluish skin discolouration
Warning signs of pulmonary embolism
The warning signs that a blood clot has travelled to the lungs can include the following:
- Rapid heart rate
- Localized chest pain with coughing
- Sudden sharp chest pain that worsens upon coughing or taking a deep breath
- Sudden shortness of breath
- Unexplained cough that brings up pink (bloody), foamy mucus.
Preventing infection
A common cause of infection after total knee replacement surgery is from bacteria that enter the bloodstream during skin infections, urinary tract infections or dental procedures. These bacteria can lodge around the knee replacement, causing an infection.
After knee replacement surgery, patients with certain risk factors may require antibiotics prior to dental work, even dental cleanings, or any surgical procedure where bacteria may enter the bloodstream. The orthopaedic surgeon and patient should discuss whether taking preventive antibiotics before dental procedures is necessary for each individual situation.
Warning signs of infection
It is crucial to notify a doctor straight away if any of the following signs of a possible knee replacement infection are developed:
- Increasing knee pain with both activity and rest
- Increasing swelling, tenderness or redness of the knee wound
- Drainage from the knee wound
- Chills
- Persistent high fever
Avoiding falls
A fall during the initial weeks after surgery can be damaging to the new knee and may result in a need for further surgery. Stairs, in particular, can be hazardous until the knee is strong and mobile. A walker, cane, crutches, handrails, or someone to assist with walking can be useful until one’s balance, flexibility and strength are improved.
The required assistive aides post-surgery and when they can be safely discontinued will be decided by one’s surgeon and physical therapist.
What are the outcomes of total knee replacement?

How different is the new knee?
Although improvement of knee motion is a goal of total knee replacement, restoration of full motion is not normal. The motion of one’s knee replacement post-surgery can be predicted by the range of motion in the knee before surgery. Majority of patients can expect to be able to almost fully straighten the replaced knee, bend it enough to climb stairs and get in and out of a car. Even though kneeling might sometimes be uncomfortable, it is not harmful.
It is not uncommon to feel some numbness in the skin surrounding the incision. Some stiffness may also be felt, particularly with excessive bending activities.
On top of that, some clicking of the metal and plastic with knee bending or walking may also be heard or felt. This is expected and normal. In fact, these differences usually fade away with time. Most patients even normally find them to be tolerable when compared with the pain and limited function pre-surgery.
Additionally, the knee replacement may activate metal detectors required for security. If the alarm is activated, simply inform the security agent of the knee replacement.
How can the knee replacement be protected?
After the surgical procedure, it is important to do the following:
Regularly participate in light exercise programs to maintain proper strength and mobility of the new knee.
Take extra precaution to avoid falls and injuries. If a bone is broken in the leg, more surgery may be required.
Ensure the dentist knows of the knee replacement. One should discuss the need for antibiotics prior to dental procedures with their orthopaedic surgeon.
Visit the orthopaedic surgeon periodically for a routine follow-up examination and X-rays. The frequency and timing of these visits will also be discussed.
How can the life of the knee implant be extended?
As of today, over 90 per cent of modern total knee replacements are still performing well 15 years after surgery. It is essential to follow instructions given by one’s orthopaedic surgeon post-surgery, take care of one’s general health and protect the knee replacement. These are all crucial ways that can contribute to the final success of the total knee replacement surgery.
Things to Do Before Undergoing Knee Replacement Surgery in Singapore
1. Look for an Experienced and Fellowship trained Orthopaedic Surgeon
A reliable surgeon should possess a strong medical background, sufficient experience, and relevant qualifications (e.g., MBBS, FRCS).
2. Informed Risk Consenting
During consultations, discuss both surgical and non-surgical options for an effective knee replacement surgery. Find out more about the pros and cons of your options.
Discuss with the surgeon about the potential of developing complications and inquire about their approach to managing them.
3. Patient Google Reviews
Patient reviews and testimonials offer real insights into a surgeon’s track record and the outcomes of their surgeries.
4. Location and Availability
Consider a surgeon with a convenient location and flexible schedules. Affiliation with a hospital or clinic offering comprehensive services, including post-surgical care and rehabilitation, is beneficial.
5. Evaluate Your Risk of Complications
Ensuring and checking the surgeons on the panel of your insurance. This is to help the patient with post-surgical follow up and claims.
FAQs about Knee Replacement Surgery
1. What is knee replacement surgery, and when is it recommended?
Knee replacement surgery, or knee arthroplasty, involves replacing damaged knee joints with artificial implants. It’s recommended for individuals with severe knee pain or limited mobility due to conditions like osteoarthritis or rheumatoid arthritis.
2. How do I know if I need knee replacement surgery?
Persistent knee pain, swelling, stiffness, and loss of function despite rehabilitation and medication are signs of a condition that may warrant knee replacement surgery. Consulting with your doctor is crucial to determine the most suitable course of action.
3. How much does knee replacement surgery cost in Singapore?
The cost depends on factors like the choice of hospital bed, the procedure fees, and the components of knee replacement. A single knee replacement surgery in a private healthcare institution generally ranges from SGD 24,000 to SGD 30,000 while similar procedures may cost about SGD 10,000 to SGD 14,000 in public hospitals. The eventual cost will also be affected by the length of your hospital stay, which is typically around 3 days following surgery.
For further information on the cost of our services at Specialist Orthopaedic Centre, please don’t hesitate to reach out and contact us.
4. What is the recovery process like after knee replacement surgery?
Recovery times can vary, but most patients are able to start walking with assistance within a day after surgery. Many patients may also choose to undergo physical therapy and rehabilitation, which play a vital role in enhancing mobility and speeding up the recovery process.
For additional insights on knee health and related topics, take a look at our published articles.
5. Are there risks associated with knee replacement surgery?
As with any surgery, knee replacement carries some risks. Although complications are rare, they can include infection, blood clots, and issues with the prosthetic implant. At Specialist Orthopaedic Centre, our surgeons will have an open discussion with you before proceeding with the surgery.
6. Is knee replacement surgery a permanent solution for knee pain?
Knee replacement surgery offers long-term relief for many individuals. However, the longevity of the artificial joint can be influenced by factors such as activity level and adherence to post-surgery care. To ensure the best possible outcome, make sure to follow your surgeon’s recommendations for recovery and maintain a healthy lifestyle.
